-
Herb overview
Safety
Not safe for pregnancy and lactation.
Not to be used in conjunction with other sedative medication.
Sustainability
Status: Low risk
Key constituents
Alkaloids
FlavonoidsQuality
Native to North America and Western Europe
Wild harvested and cultivatedKey actions
Sedative
Anxiolytic
Nervine
RelaxantKey indications
Insomnia
Anxiety
Stress
ADHDKey energetics
Cool
Relaxing
SweetPreperation and dosage
Aerial parts
Dried herb: <8 g per day
Fluid extract: <8 ml per day
-
How does it feel?
Passionflower has a delicate herby taste, with mildly sour and sweet tones. The sourness can be primarily perceived by the receptors on the sides of the tongue. The infusion of the dried herb is refreshingly pleasant, smooth and easy to drink.
The physical sensation after ingesting a passionflower infusion is one of deep calm. The tea has a smooth, rich texture which adds to its nurturing and nourishing quality. The calming nervine effects of this herb are often felt soon after taking. The aromatic compounds directly influence GABAergic neurotransmission, reducing nervous activity to soothe and settle the mind and body.
-
Into the heart of passionflower

Passionflower (Passiflora incarnata) Passionflower is deemed to be mildly cooling in the understanding of Western herbal energetics. This cooling action reduces heat, excitation and overstimulation in the cells (3). Whilst passionflower is less obviously sour than other medicinal herbs , it does have a notable sour taste. This cooling action is often seen in plants that have a sour taste profile. Herbs like sorrel (Rumex acetosa) and lemon balm (Melissa officinalis) also fit in this category of non-fruiting sour relaxants whose actions may be well applied for this type of nervous excitability.
In Ayurveda, passionflower is thought to decrease pitta and kapha. It also moves obstructed vata. It is said that when used in excess, it may increase vata, so it is likely best to use with caution for individuals with a high vata constitution (4).
Similar to Ayurveda, traditional Chinese medicine (TCM) has its own unique system of understanding health balance and disease. TCM understands passionflower to be of a calming nature, relieving anxiety and soothing the spirit. It also tonifies Heart yin (put simply, yin translates as a restorative energy that allows the body and mind to slow down, rest and relax), whilst also clearing internal wind. Internal wind may be indicated by the presence of spasms, pain and seizures arising from hyperactive Liver yang (yang refers to active energy, heat, movement and power) (5).
In the energetics of the eclectics, passionflower is understood to be best adapted to debility and nervous irritability. It is specifically indicated for irritation of the brain and nervous system with atony. This herb is appropriate for those whose sleep is affected by overwork, worry and exhaustion. In addition, convulsions, hysteria and oppressed breathing may be present (6).
-
What practitioners say
 Nervous system
Nervous systemPassionflower has a marked sedative effect on the central nervous system. It is often used by herbalists to treat anxiety, restlessness and other mental health conditions. It has been shown to improve symptoms in people with attention deficit disorder (ADD) as well as in alleviating withdrawal symptoms in people recovering from conventional and recreational drug addictions (12,13,14).
Passionflower is an excellent remedy for insomnia. It works most effectively when taken in the evening to support the transition into sleep. It is well known to induce a restful sleep without a feeling of grogginess the next day that can often accompany sedatives (15,16).
Furthermore, passionflower can be applied to spasmodic conditions, such as the spasmodic muscular convulsions seen in epilepsy (1,15). It is also referenced for use in Parkinson’s disease (16). The antispasmodic actions also indicate its use in the treatment of neuralgia and pain from shingles (16).
As a sedative, passionflower can be used in the acute treatment of mania and also for panic attacks, but it is also safe to use for chronic anxiety. Passionflower is a more gentle sedative than other herbs like valerian and hops (2).
Digestive system
Passionflower may be applied in spasmodic conditions of the digestive system, particularly where these are linked to stress and tension such as with irritable bowel syndrome (IBS). This herb is antispasmodic, meaning that it can easily relax tension held in the digestive tract such as in flatulence and intestinal spasm. This spasmodic state can also be seen in conditions such as reflux, colic and dysentery (1,16).
Cardiovascular system
Passionflower additionally acts as an antihypertensive to reduce high blood pressure and prevent tachycardia, particularly where the cause is stress. Traditionally, it has been applied to reduce palpitations. This mechanism is likely due to its effect on the nervous system in reducing the stress response, as opposed to a specific cardiac mechanism (1,3).
Respiratory system
Passionflower can be useful in the treatment of spasmodic asthma and whooping cough (2,16). As a herb with powerful antispasmodic actions, passionflower can be applied where these conditions leave a patient with persistent tension in the lungs and diaphragm that leads to spasmodic coughing (2,16).
-
Passionflower research

Passionflower (Passiflora incarnata) Passionflower in the treatment of generalized anxiety: A pilot double-blind randomised controlled trial with oxazepam
A double-blind randomised control trial was carried out to compare the efficacy of Passiflora incarnata extract with oxazepam (an anti-anxiety and insomnia pharmaceutical medication) in the treatment of generalised anxiety disorder.
The study was carried out on outpatients with a generalised anxiety diagnosis. Patients were randomly allocated — with 18 participants receiving the passionflower extract at 45 drops per day, 18 in the placebo tablet group, and 18 to receive oxazepam at 30 mg per day plus placebo drops over a four week trial period.
The results show that passionflower extract and oxazepam are equally as effective in the treatment of generalised anxiety disorder. However, subjects taking oxazepam displayed significantly more problems relating to impairment of job performance. The study concludes that Passionflower is effective for the management of generalized anxiety disorder. Passionflower holds the advantage over oxazepam with its low incidence of impairment of job performance and side effects (16).
Passiflora incarnata in neuropsychiatric disorders—A systematic review
A systematic review was carried out on nine different clinical trials where passionflower is used in the treatment of psychiatric disorders. The review includes a number of studies where passionflower was used in clinical trials to assess its efficacy for anxiety. Some of these studies focused on preoperative and pre-spinal anaesthesia anxiety and also for anxiety related to dental procedures.
The results across each study showed that passionflower was safe and effective for reducing anxiety. This includes the case of conscious sedation in adult patients. Passionflower was found to significantly contribute to reducing pre-procedural anxiety. A very low incidence of side effects was reported, however, a study where passionflower was used in preoperative anxiety found that psychomotor functions were impaired 30 minutes after extubation (17).
The same review discusses the results of a study where the effects of passionflower were compared to midazolam for bilateral extraction of the mandibular third molars. The anxiolytic action of both substances used in the study was similar. Among the subjects in the midazolam group, 20% reported significant memory loss, while none of the patients receiving passionflower reported such an experience. The midaxolam group reported a higher incidence of drowsiness (17).
The review concludes with a theme of strong evidence to support that passionflower is able to alleviate some symptoms of neuropsychiatric origin. The anxiolytic effect of passionflower is comparable to the drugs oxazepam or midazolam. However, passionflower holds the advantage of having little to no adverse reactions, such as including memory loss or collapse of psychometric functions as often seen with its pharmaceutical equivalents. Consequently, passionflower offers a safe and effective medicine to reduce stress reactivity, insomnia, anxiety, and depression-like behaviours (17).
Randomised, double-blind, placebo-controlled, clinical study of Passiflora incarnata in participants with stress and sleep problems
This randomised, double blind, placebo controlled clinical study was carried out to evaluate the effect of a passionflower extract on participants with stress and sleep issues. Participants were randomly divided into two groups, one (32 people) to receive 600 mg of passionflower at bedtime and the other (33 people) placebo group to receive placebo capsules. The study was carried out over a 30 day time period, with assessments carried out on day 1, 15 and 30.
Results showed a significant reduction on the Perceived Stress Scale (PSS) in the passionflower group vs placebo, an increase in total sleep time in the passionflower group as well as a notable increase in overall psychological health in the passionflower group. There were no adverse effects reported, suggesting passionflower is an effective remedy in reducing stress levels and supporting sleep (18).
Passiflora incarnata in the treatment of attention-deficit hyperactivity disorder in children and adolescents
In an eight-week, double-blind, randomised clinical trial the effectiveness of passionflower in treatment of ADHD was carried out on a group of 34 children aged between the ages of 6 to13 years old. Subjects in the treatment group were given 0.04 mg passionflower tablets twice daily whilst the control received methylphenidate (an ADHD medication) at 1 mg twice daily. Both treatment groups demonstrated significant clinical benefits over the period of treatment as assessed by both parents and teachers. The study concludes that “passionflower may be a novel therapeutic agent for the treatment of ADHD” (12).
Research into passionflower’s effects on psychiatric disorders is promising, however larger scale clinical trials and studies are required to add more weight to the evidence base.
-
Historical use of passionflower

Passionflower (Passiflora incarnata) In Grieves’ A Modern Herbal written originally in 1931, the traditional uses of passionflower are understood to be due to a combined effect as a nervous system depressant. She described this mechanism to be specifically affecting descending motor pathways (7).
Historical records show that the Aztecs used passionflower for its medicinal benefits, including for the treatment of urinary tract disorders, bone fractures, and skin contusions.
Traditionally, Native Americans used passionflower as a sedative (8).
Nicolas Monardes, a Spanish doctor working in Peru, was the first European to bring passionflower to Europe after learningof its medicinal uses from the Indigenous peoples of South America in 1569. Subsequently, passionflower became widely cultivated and used in European folk medicine (9).
North American physicians prescribed passionflower for its effects on spasmodic conditions, such as seizures and epilepsy. In the early 20th century, European physicians were understood to have used passionflower to treat anxiety and mild sleep disorders (10).
-
Passionflower’s herbal actions
Herbal actions describe therapeutic changes that occur in the body in response to taking a herb. These actions are used to express how a herb physiologically influences cells, tissues, organs or systems. Clinical observations are traditionally what have defined these actions: an increase in urine output, diuretic; improved wound healing, vulnerary; or a reduction in fever, antipyretic. These descriptors too have become a means to group herbs by their effects on the body — herbs with a nervine action have become the nervines, herbs with a bitter action are the bitters. Recognising herbs as members of these groups provides a preliminary familiarity with their mechanisms from which to then develop an understanding of their affinities and nuance and discern their clinical significance.
-
Passionflower’s energetic qualities
Herbal energetics are the descriptions Herbalists have given to plants, mushrooms, lichens, foods, and some minerals based on the direct experience of how they taste, feel, and work in the body. All traditional health systems use these principles to explain how the environment we live in and absorb, impacts our health. Find out more about traditional energetic actions in our article “An introduction to herbal energetics“.
-
What can I use passionflower for?

Passionflower (Passiflora incarnata) Passionflower is a key remedy for reducing anxiety. This herb can be used to support multiple symptoms of anxiety. A typical indication for passionflower is where anxiety is accompanied by racing and repetitive thoughts. Symptoms may also present with agitation, restlessness, spasms, neuralgic pain, headaches, palpitations and feelings of panic. Passionflower can be applied to help with any of these symptoms as it facilitates a feeling of calm and relaxation (1).
Passionflower works directly on the central nervous system, alleviating overactivity. Passionflower brings peace to the nervous system and allows one to function from a place of calm, regaining a sense of confidence and control (2).
The grounding effects of passionflower are especially helpful where these types of presentations are accompanied by sleep disturbances, such as insomnia. It is a gentle relaxant and a mild hypnotic (2).
Passionflower is also sometimes used to alleviate nervous irritability that can accompany weaning off from pharmaceutical sedatives or anxiety medications. Recovery from alcohol and drug addictions may also be supported by passionflower via the same mechanism. For this application, it may be combined with other nervine sedative herbs, such as hops (Humulus lupulus) and valerian (Valeriana officinalis) (1). Furthermore, where digestive symptoms arise from stress and tension, passionflower may be used as a stomach relaxant and for symptoms of indigestion, particularly (2).
-
Did you know?
The name passionflower refers to the ‘passion of christ’. It was thought to symbolise events in the last hours of the life of Jesus Christ. Symbolically the corona or flower was thought to represent the crown of thorns, the styles represent the nails used in the crucifixion, the stamens represent the five wounds, and the five sepals and five petals represent 10 of the Apostles — all but Judas and Peter (7).
-
Botanical description
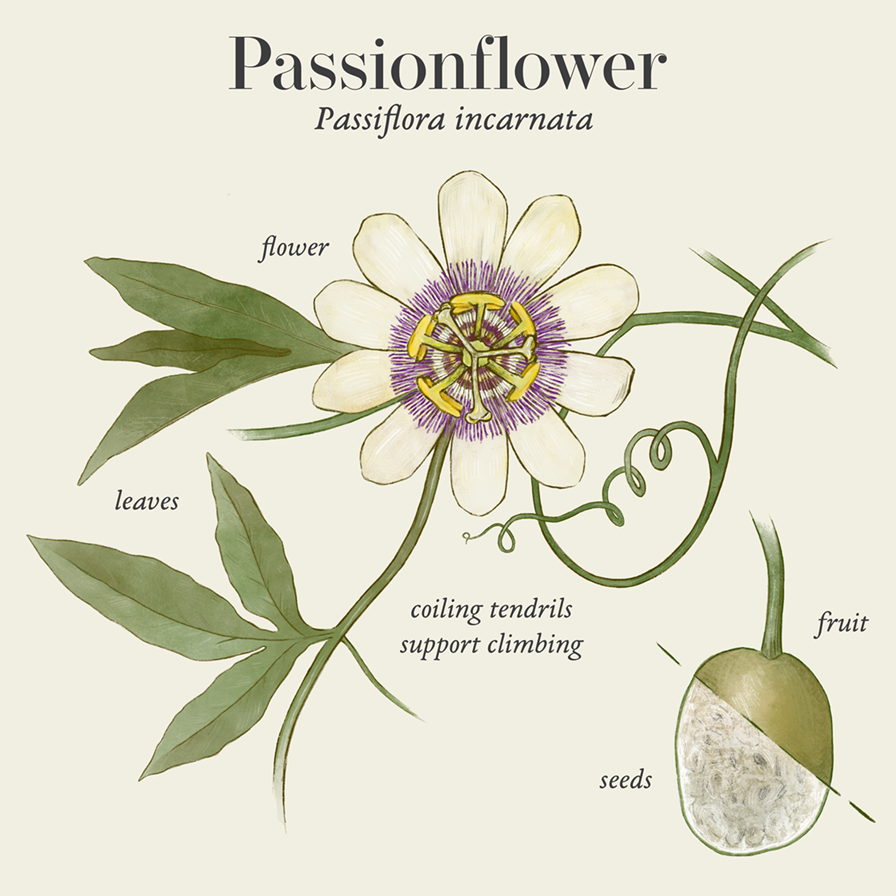
Passiflora incarnata is a sub species in the Passifloraceae genus which contains more than 550 different species. It is a perennial climbing vine, with extending tendrils.
The leaves are alternate, serrate and three lobed reaching to between 10–15 cm long.
The flowers contain five sepals and five petals and can be white, purple, pink or blue in colour. The corona contains pink or purple filaments. The edible yellow fruit grows up to 5 cm long.
The plant flowers in summer and autumn in the northern hemisphere (19).
-
Common names
- Maypop
- Passion vine
- Granadilla
- Water lemon
- Maracuya
- Flor de la pasion
- Fleur de la passion
-
Habitat
Passionflower is native to the southeastern United States, Central and South America. It typically grows in sandy soils, roadsides, prairies, plains, meadows, pastures, woodland edges, streams and riverbanks (20).
-
How to grow passionflower
Passionflower is a hardy plant that is easy to grow. It blooms over a long period from early summer until autumn. It grows best in any fertile, well-drained soil in a sunny, sheltered position in the garden. The following advice is focused on how to grow in small potted plants.
Plants for sale are usually of flowering size and available in 1 or 2 litre pots
Plant passionflower in the spring after the cold weather has passed (typically late May/early June). Passionflower planted in the garden border will produce the best growth and flowers when in a sunny, sheltered position away from cold drying winds. A south- or west- facing fence or wall is ideal.
Passionflower will climb by means of their tendrils and need to be planted and trained against a trellis or horizontally-wired fence or wall on which the tendrils can cling. The growing area needs to permit up to 10 m of growth.
Water passionflower once a week during dry spells and container plants as soon as the surface of the soil looks dry. Flowering may reduce in particularly dry spells.
The roots can be fertilised in the spring using a general fertiliser. During the winter, no feeding is required as the plant will be dormant (21).

-
Herbal preparation of passionflower
- Tincture
- Capsules
- Infusion
-
Plant parts used
Aerial parts
-
Dosage
- Tincture (1:5 | 45%): Between 1–8 ml per day divided into two or three equal doses (16)
- Fluid extract (1:1 | 25%): 1.5–8 ml per day (16)
- Infusion/decoction: Add 1–2 tsp of dried herb to a mug of water, steeping for 15 minutes. After straining, drink passionflower tea up to three times a day (15,16).
-
Constituents
- Indole alkaloids (up to 9%): Harmene is the primary alkaloid, along with, harman, halo, harmaline, harmalol, passiflorine
- Flavonoids (0.8–2.5%): Flavone C-glycosides, apigenin (up to 2.5%) luteolin, rutin, homoorientin, orientinkaempferol, quercetin, saponarin and isovitexin
- Phenolics: Caffeic acid, chlorogenic acid, ferulic acid
- Fatty acids
- Sterols: Passicol is a polyacetylene and is antimicrobial
- Volatile oils
- Vitamins: K (15,16)
-
Passionflower recipe
Peace tea
This delicious passionflower peace tea is made with equal parts of passionflower, lavender, limeflower and chamomile.
Ingredients
Equal parts of:
- Passionflower
- Limeflower (Tilia spp.)
- Lavender (Lavandula angustifolia)
- Chamomile (Matricaria chamomilla)
How to make passionflower tea
- Mix equal parts of the dried herbs to the approximate weight of 5–10 g (or 3–4 teaspoons. Steep in hot water in a teapot for up to 15 minutes. Then strain the infusion into your favourite mug. Drink throughout the day.
- This blend of gently relaxing and aromatic herbs will help bring a sense of calm and relaxation in mind, body and spirit.

-
Safety
Passionflower is generally referenced as unsafe to take during pregnancy and lactation. If you are pregnant or breastfeeding it is best to consult with a clinical herbalist before taking this herb (15,16,22).
-
Interactions
Passionflower may increase the effects of prescription sedatives, antispasmodics and anxiolytics; it is best to consult a herbal practitioner if you are taking any of these medications (15,16,22). This is, however, mostly theoretical and no interactions have been reported to date.
Passionflower should not be taken alongside the older types of anti-depressants called monoamine oxidase inhibitors (MAOIs) (15,16,22).
-
Contraindications
None known (15,16,22).
-
Sustainability status of passionflower

According to NatureServe, passionflower was last assessed for its endangered rating in 1994. It was then classified as stable in many areas of its native habitat across the United States of America.
It also states the global reassessment is in need of review (23). It is not listed on the IUCN redlist of threatened species, and is not considered to be at risk as it an adaptable plant that grows prolifically in the right conditions (24).
Read our article on Herbal quality & safety: What to know before you buy and Sustainable sourcing of herbs to learn more about what to look for and questions to ask suppliers about sustainability.


-
Quality control
Passionflower is both wild harvested and cultivated for medicinal uses. There are no known contamination or adulteration risks if sourced from a reputable supplier (16).
-
References
- MENZIES-TRULL C. HERBAL MEDICINE KEYS to PHYSIOMEDICALISM INCLUDING PHARMACOPOEIA.; 2022.
- Mcintyre A. Complete Herbal Tutor : The Definitive Guide to the Principles and Practices of Herbal Medicine (Second Edition). Aeon Books Limited; 2019.
- Wood M. The Practice of Traditional Western Herbalism : Basic Doctrine, Energetics, and Classification. North Atlantic Books, Cop; 2004.
- Pole S. Ayurvedic Medicine : The Principles of Traditional Practice. Singing Dragon, Cop; 2013.
- Holmes P. The Energetics of Western Herbs : Treatment Strategies Integrating Western and Oriental Herbal Medicine. Snow Lotus Press; 2007.
- King J. The American Eclectic Dispensatory. Moore, Wilstach, Keys, & Co; 1856.
- Grieve M. A Modern Herbal | Passion Flower. botanical.com. Published 2025. Accessed March 31, 2021. https://botanical.com/botanical/mgmh/p/pasflo14.html
- Miroddi M, Calapai G, Navarra M, Minciullo PL, Gangemi S. Passiflora incarnata L.: Ethnopharmacology, clinical application, safety and evaluation of clinical trials. Journal of Ethnopharmacology. 2013;150(3):791-804. https://doi.org/10.1016/j.jep.2013.09.047
- Ubrizsy A, Heniger J. CAROLUS CLUSIUS AND AMERICAN PLANTS. TAXON. 1983;32(3):424-435. https://doi.org/10.2307/1221499
- British Herbal Medicine Association. Passion Flower | British Herbal Medicine Association. Bhma.info. Published 2025. Accessed December 18, 2025. https://bhma.info/indications/sleep-problems-and-fatigue/passion-flower/
- Winston D, Maimes S. Adaptogens : Herbs for Strength, Stamina, and Stress Relief. Healing Arts Press; 2007.
- Akhondzadeh S, Mohammadi M, Momeni F. Passiflora incarnata in the treatment of attention-deficit hyperactivity disorder in children and adolescents. Therapy. 2005;2(4):609-614. https://doi.org/10.1586/14750708.2.4.609
- Anheyer D, Lauche R, Schumann D, Dobos G, Cramer H. Herbal medicines in children with attention deficit hyperactivity disorder (ADHD): A systematic review. Complementary Therapies in Medicine. 2017;30:14-23. https://doi.org/10.1016/j.ctim.2016.11.004
- Akhondzadeh S, Kashani L, Mobaseri M, Hosseini SH, Nikzad S, Khani M. Passionflower in the treatment of opiates withdrawal: a double-blind randomized controlled trial. Journal of Clinical Pharmacy and Therapeutics. 2001;26(5):369-373. https://doi.org/10.1046/j.1365-2710.2001.00366.x
- Fisher C. Materia Medica of Western Herbs. Aeon Books; 2018.
- Hoffmann D. Medical Herbalism: The Science and Practice of Herbal Medicine. Healing Arts Press; 2003.
- Akhondzadeh S, Naghavi HR, Vazirian M, Shayeganpour A, Rashidi H, Khani M. Passionflower in the treatment of generalized anxiety: a pilot double-blind randomized controlled trial with oxazepam. Journal of Clinical Pharmacy and Therapeutics. 2001;26(5):363-367. https://doi.org/10.1046/j.1365-2710.2001.00367.x
- Harit MK, Mundhe N, Tamoli S, et al. Randomized, Double-Blind, Placebo-Controlled, Clinical Study of Passiflora incarnata in Participants With Stress and Sleep Problems. Curēus. Published online March 20, 2024. https://doi.org/10.7759/cureus.56530
- Prenner G. A passion for passion flowers | Kew. www.kew.org. Published 2025. Accessed April 11, 2021. https://www.kew.org/read-and-watch/passion-for-passion-flowers
- United States Department of Agriculture. PURPLE PASSIONFLOWER Passiflora Incarnata L. Plant Symbol = PAIN6.; 2025. https://plants.usda.gov/DocumentLibrary/plantguide/pdf/pg_pain6.pdf
- RHS. How to grow passion flowers / RHS Gardening. www.rhs.org.uk. Published 2025. Accessed May 4, 2023. https://www.rhs.org.uk/plants/passion-flower/growing-guide
- Natural Medicines Database. Passionflower. Therapeuticresearch.com. Published 2025. Accessed December 18, 2025. https://naturalmedicines.therapeuticresearch.com/Data/ProMonographs/Passion-Flower#safety
- NatureServe Explorer. Passiflora incarnata. explorer.natureserve.org. Published 2025. Accessed December 6, 2022. https://explorer.natureserve.org/Taxon/ELEMENT_GLOBAL.2.154895/Passiflora_incarnata
- IUCN Redlist. Passiflora incarnata. IUCN Red List of Threatened Species. Published 2025. Accessed December 18, 2025. https://www.iucnredlist.org/search?query=passiflora%20incarnata&searchType=species